Auteur: Joe Hylton, MA, BSRT, RRT-ACCS/NPS, NRP, FAARC, FCCM, spécialiste en applications cliniques, Hamilton Medical Inc.
Date: 15.07.2021
Il est clairement établi que le métabolisme, la perfusion et une bonne fonction pulmonaire sont essentiels au transport et à une élimination efficaces du CO2 (1). Les changements de l'état métabolique, de la perfusion ou de la fonction pulmonaire du patient peuvent affecter l'élimination du CO2, parfois de manière dramatique.

La capnographie sous formes d'ondes de base donne aux médecins la possibilité de surveiller en continu la pression partielle de CO2 de fin d'expiration (PetCO2) et d'identifier potentiellement les changements de l'état général du patient ventilé mécaniquement.
Les ventilateurs Hamilton Medical qui utilisent le monitorage de CO2 «mainstream » ou « sidestream » offrent une forme d'ondes PetCO2 intégrée et fournissent aux médecins la possibilité de surveiller la PetCO2. Le médecin peut comparer en temps réel la forme d'ondes de capnographie avec les formes d'ondes de débit et de pression, pour permettre éventuellement l'identification de problèmes susceptibles de survenir (augmentation de la résistance des voies aériennes, augmentation de l'espace mort, fuites des voies aériennes, par ex.) (
Lorsque vous commencez à prendre la mesure du CO2, il est préférable d'obtenir un gaz du sang artériel, afin de comparer la PaCO2 avec la PetCO2. Dans le cadre d'une physiologie normale, le gradient PaCO2-PetCO2 doit être de 2-5 mmHg. Les plages normales acceptables pour la PetCO2 sont identiques à celles du gaz du sang artériel, 35-45 mmHg. Si le gradient dépasse 5 mmHg, le médecin doit évaluer tout facteur physiologique et matériel possible, susceptible d'affecter la mesure de la PetCO2. Des pathologies telles qu'un SDRA, une insuffisance cardiaque/un œdème pulmonaire, de l'asthme, une BPCO/un emphysème, des conditions de perfusion faible (choc/hypotension, sepsis, infarctus du myocarde, insuffisance cardiaque) et une embolie pulmonaire peuvent contribuer à un gradient PaCO2-PetCO2 amplifié.
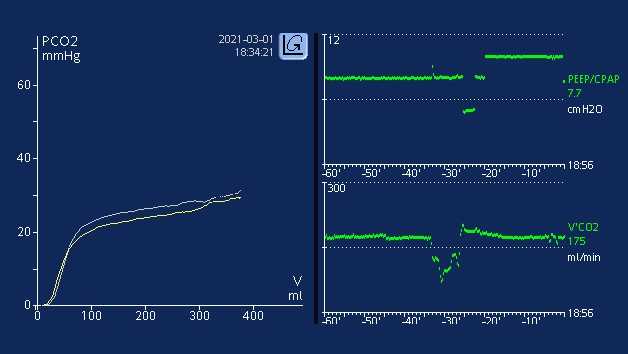
Corriger un décalage ventilation-perfusion, par exemple en inversant le choc/l'hypotension (en réduisant l'espace mort), ou utiliser une manœuvre de recrutement et ajuster la PEP chez un patient SDRA (en réduisant le shunt) peut diminuer le gradient PaCO2-PetCO2 dans une plage plus acceptable (
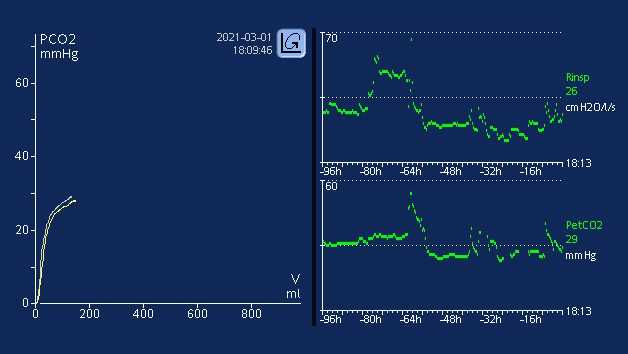
Afficher une tendance de PetCO2 et de V’CO2 est un bon moyen de détecter les éventuels changements de l'état du patient. Un changement de la température du patient (hyperthermie/fièvre par ex.) ou une diminution du débit cardiaque/de la pression sanguine (bradycardie, choc neurogénique/hémorragique, par ex.) peut provoquer d'éventuels changements dans l'élimination du CO2. La capacité à dégager une tendance de PetCO2 et de V’CO2 peut permettre au médecin d'identifier plus tôt d'éventuels changements ou à l'équipe de mieux identifier la survenue d'un événement. La capacité des médecins à intervenir lors de la survenue éventuelle d'événements critiques ou la capacité à mieux identifier la survenue d'un événement peut fournir des informations cruciales pour les résultats du patient. L'affichage d'une tendance de PetCO2 et de V’CO2 peut se révéler être un outil de diagnostic efficace pour démontrer le bénéfice de manœuvres de réanimation (remplacement du volume vasculaire, amélioration de la résistance vasculaire systémique pour améliorer l'espace mort), ou lorsque des manœuvres de recrutement et un titrage de la PEP sont effectués pour éventuellement diminuer le phénomène de shunt. Les ventilateurs Hamilton Medical donnent aux médecins la possibilité d'afficher une tendance des paramètres de monitorage de CO2 suivants sur des périodes allant jusqu'à 96 heures (sur les HAMILTON-G5/S1 ; jusqu'à 72 heures sur les HAMILTON-C1/C3/C6/T1) : PetCO2, V‘CO2, FetCO2, VeCO2, ViCO2, VTE/Valv, Vds, VD/Vt et penteCO2. Ces paramètres peuvent être tracés en fonction de tout autre paramètre de monitorage disponible. L'affichage des tendances peut se faire en temps réel via les vues des panneaux intelligents du Ventilation Cockpit.
Citations complètes ci-dessous : (


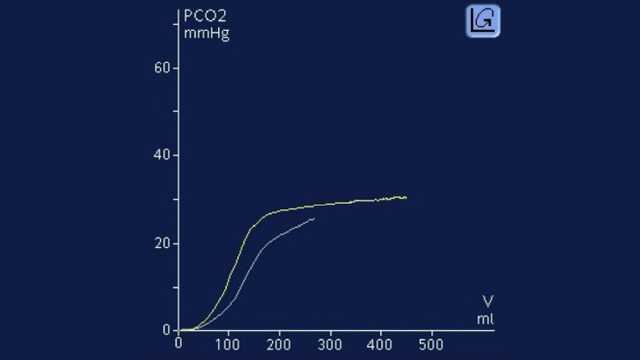
Apprenez à interpréter un capnogramme volumétrique et découvrez les avantages et les applications cliniques de la capnographie volumétrique. Inclut un auto-test !