
Author: Simon Franz
Date of first publication: 14.07.2017
A common question asked by users of HAMILTON-C1/T1/MR1 ventilators is how to measure/calculate Pplateau with their device.

Even if the idea of a “safe” plateau pressure is already being questioned, it is still standard of care to use it for tailoring lung-protective ventilation in acute respiratory distress (ARDS) patients
Due to the valveless pneumatics in the HAMILTON-C1/T1/MR1 ventilators, it is not possible to obtain the Pplateau by performing an inspiratory hold maneuver. Nevertheless, Pplateau is still available as a monitoring parameter and maybe displayed depending on your ventilator's software.
| HAMILTON-C1/T1/MR1 SW < v2.2.0 | HAMILTON-C1/T1/MR1 SW ≥ v2.2.0 |
|---|---|
| End-inspiratory pressure always displayed as Pplateau. Please consider that if an end-inspiratory flow is present, the Pplateau displayed is higher than the actual Pplateau. | Pplateau is only displayed if the end-inspiratory flow is close to zero. The Pplateau displayed can still be higher than the actual Pplateau. |
A possible workaround for calculating Pplateau in situations where the end-inspiratory flow is not close to zero or the pressure measured end-inspiratory seems inaccurate:
This calculation is dependent on an accurate Cstat measurement, which means there is no significant patient effort occurring. Pinsp should be at least ~10cmH2O.
Pplateau = (VTE ml / Cstat ml/cmH2O) + PEEP cmH2O
Example
VTE: 450 ml; Cstat: 50 ml/cmH2O; PEEP: 8 cmH2O
(450 ml / 50 ml/cmH2O) + 8 cmH2O = 17 cmH2O
Pplateau = 17 cmH2O
∆P = 9 cmH2O
Another benefit is that you get the ∆P as a side product of your calculations. ∆P is strongly associated with survival in ADRS patients and may therefore be the more interesting parameter
Relevant devices: HAMILTON-C1/T1/MR1 (all software versions)

ARDS is characterized by lung collapse and consolidation leaving just a small portion of aerated lung remaining, which is at risk of ventilator-induced lung injuries (baby-lung concept).
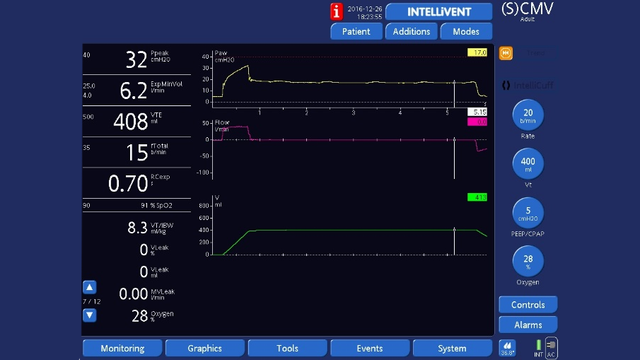
Airway driving pressure is associated with clinical outcomes in ARDS, post-surgical, and normal-lung patients, and is a measure of the strain applied to the respiratory system and the risk of ventilator-induced lung injuries. Evidence suggests we should keep driving pressure below 14 cmH2O. But how can we measure it?