Autore: Dr. Jean-Michel Arnal, intensivista senior, Hôpital Sainte Musse, Tolone, Francia
Data: 19.10.2018
Last change: 09.09.2020
FormattingUno studio fisiologico recente ha dimostrato che la pressione esofagea rappresenta una stima della pressione pleurica nella zona centrale del torace a tutti i livelli di PEEP. Una misurazione assoluta della pressione esofagea è quindi utile per impostare la PEEP e monitorare la pressione transpolmonare.

Come si misura correttamente la pressione esofagea?
È necessario posizionare e gonfiare correttamente il palloncino esofageo, quindi verificarne il posizionamento.
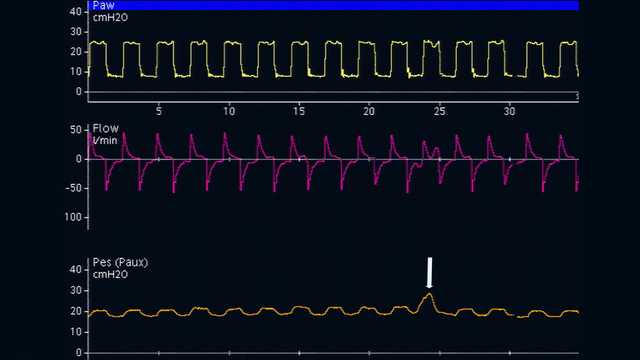
La posizione ottimale per il palloncino esofageo è nel terzo inferiore dell'esofago, a una distanza di 35-45 cm dalle narici. Con il paziente in posizione semi-supina, per prima cosa si inserisce il palloncino sgonfio nello stomaco, situato a circa 50-60 cm dalle narici. Si gonfia quindi il palloncino fino a un volume standard (1 ml per un catetere CooperSurgical e 4 ml per un catetere NutriVent). La pressione gastrica è caratterizzata da una deflessione positiva durante l'inspirazione sia nei pazienti passivi sia in quelli che respirano spontaneamente. Si verifica che il palloncino sia in posizione gastrica esercitando delicatamente una compressione epigastrica manuale che corrisponde a un aumento immediato della pressione (vedere la Figura 1).

Occorre quindi tirare indietro delicatamente il catetere esofageo con il palloncino gonfio per posizionare il palloncino nel terzo inferiore dell'esofago. Quando si passa dalla pressione gastrica (vedere la Figura 2) a quella esofagea (vedere la Figura 3), la linea basale della curva di pressione cambia e compaiono le oscillazioni cardiache.
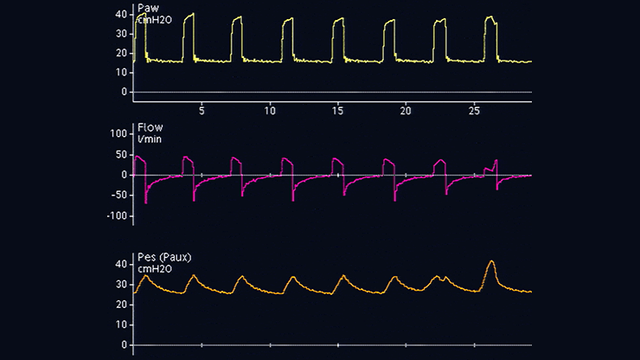
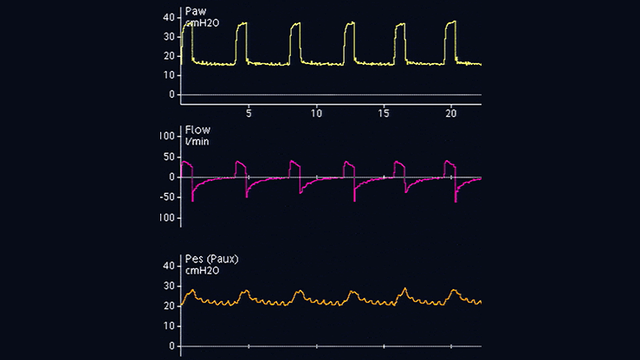
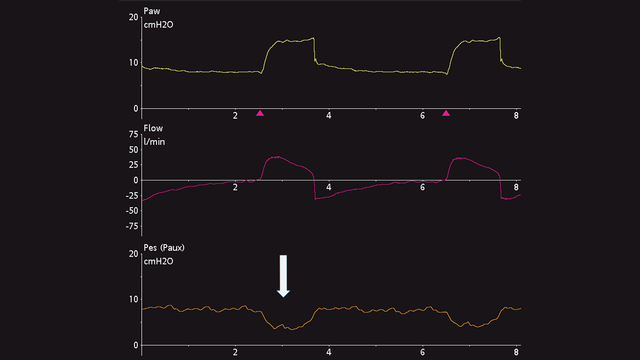
Le deflessioni nella curva della pressione esofagea sono positive durante l'inspirazione nei pazienti passivi (vedere la Figura 4), mentre sono negative nei pazienti che respirano spontaneamente (vedere la Figura 5). Se le oscillazioni cardiache distorcono il segnale della pressione esofagea, è possibile tirare indietro il catetere ancora di 2-5 cm.
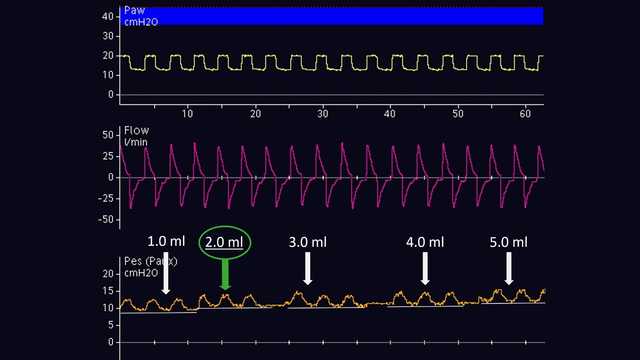
Il volume di aria necessario per un gonfiaggio adeguato del palloncino deve essere determinato su base individuale. È possibile fare questa operazione solo nei pazienti passivi. Secondo il metodo proposto da Mojoli et al. (2016), se si utilizza un catetere CooperSurgical il palloncino deve essere gonfiato da 0,5 a 3 ml con incrementi graduali da 0,5 ml, mentre se si utilizza un catetere NutriVent il palloncino deve essere gonfiato da 1 a 8 ml con incrementi graduali da 1 ml (vedere la Figura 6). Durante il progressivo gonfiaggio del palloncino, la linea basale della pressione esofagea sale e l'ampiezza della deflessione nella curva della pressione esofagea cambia. Il volume di gonfiaggio adeguato è quello associato alla deflessione più ampia nella curva della pressione esofagea. Se l'ampiezza della deflessione nella pressione esofagea è la stessa per due diversi volumi di gonfiaggio, è opportuno scegliere il volume di gonfiaggio più basso.
Dopo aver posizionato il palloncino correttamente nell'esofago e dopo averlo gonfiato, occorre eseguire la verifica con un test di occlusione. L'idea di base è di chiudere le vie aeree al termine dell'espirazione per modificare la pressione delle vie aeree, quindi verificare che la pressione esofagea registri una variazione equivalente.
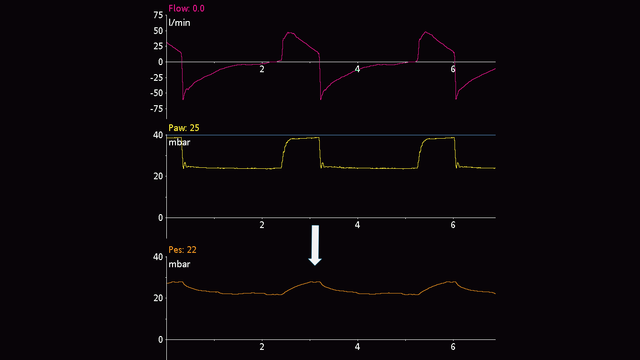
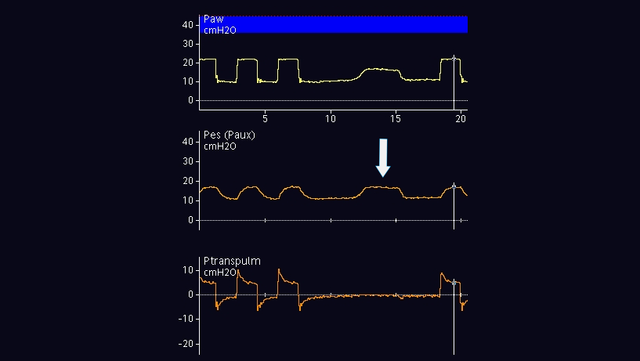
Nei pazienti passivi è possibile effettuare un'occlusione a fine espirazione. Quando la valvola espiratoria è chiusa, applicare una compressione manuale esterna su entrambi i lati della gabbia toracica: si osserva una deflessione positiva della pressione delle vie aeree e della pressione esofagea. L'entità dell'aumento deve essere la stessa nella pressione delle vie aeree e in quella esofagea. In altre parole, la pressione transpolmonare non deve subire variazioni (vedere la Figura 7).
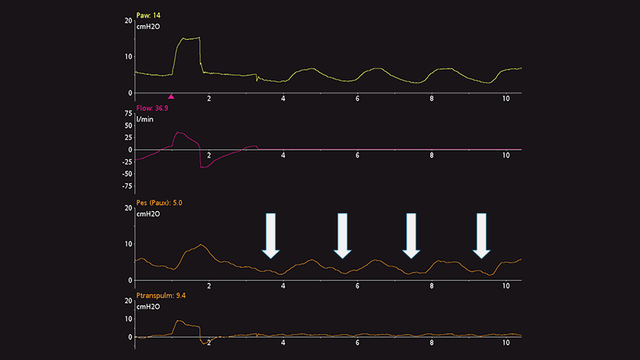
Anche nei pazienti attivi il test di occlusione dinamica si basa su un'occlusione a fine espirazione. Non è necessario comprimere il torace manualmente, poiché il paziente compie uno sforzo inspiratorio spontaneo durante l'occlusione. Si crea così una deflessione negativa nelle curve della pressione delle vie aeree e della pressione esofagea. L'entità della diminuzione registrata nella pressione delle vie aeree e in quella esofagea deve essere la stessa, ovvero la pressione transpolmonare non deve subire variazioni (vedere la Figura 8).
Se si desidera monitorare in modo continuo la pressione esofagea, è importante rivalutare il corretto posizionamento e il volume di gonfiaggio.
Citazioni complete a fondo pagina: (

Raccomandazioni comprovate in ambiente clinico su cosa fare e non fare quando si utilizza la pressione esofagea nei pazienti con ARDS.